Denials management is a structured process used by healthcare organizations to identify, analyze, correct, and prevent claim denials. It plays a critical role in revenue cycle performance. When claims are denied, payment is delayed or lost. Without a clear strategy, denials can weaken financial stability and increase administrative burden.
According to the Centers for Medicare and Medicaid Services, improper payments in federal healthcare programs continue to be a major concern each year, often linked to documentation and billing errors. This highlights why organized denials management is essential for compliance and reimbursement accuracy.
Understanding a Medical Denial
A medical denial occurs when a payer refuses to reimburse a claim after review. This decision may be partial or full. It happens for several reasons, including missing documentation, coding errors, eligibility issues, or a lack of authorization.
In simple terms, the provider performed the service, submitted the claim, and expected payment. The payer reviewed the claim and determined it did not meet specific requirements.
Denials are not always final. Many can be corrected and resubmitted if handled properly.
Why Denials Management Matters in Healthcare
Denials management in healthcare is not just about fixing rejected claims. It is about preventing repeat errors and strengthening the entire revenue cycle.
The American Hospital Association has reported that administrative burdens and payer-related inefficiencies continue to strain hospital resources. Claim denials contribute significantly to this strain. Each denied claim requires staff time, review, correction, and follow-up.
Without a structured approach, organizations lose revenue and productivity.
The Denial Lifecycle in Revenue Cycle Management
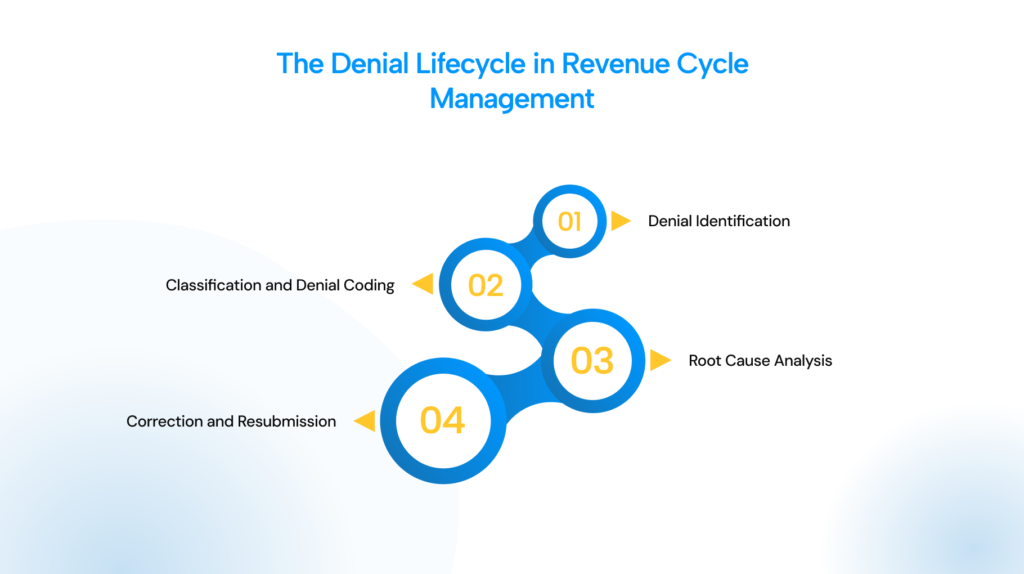
Denial management in RCM follows a clear lifecycle. It begins when a payer issues a denial and ends when the issue is resolved or written off.
Denial Identification
The first step is recognizing that a claim has been denied. This usually happens through remittance advice or electronic reports. Billing teams must review denial codes and payer explanations carefully.
Classification and Denial Coding
Denial coding categorizes the reason for denial. This step helps identify patterns. For example, repeated eligibility errors may point to front-end registration problems. Accurate categorization supports better analysis and prevention planning.
Root Cause Analysis
This stage focuses on why the denial occurred. Was the documentation incomplete?
Was the diagnosis code incorrect? Was authorization missing?
Research from the Office of Inspector General frequently emphasizes documentation deficiencies as a root cause of payment errors in federal healthcare audits. Identifying these causes early reduces repeat denials.
Correction and Resubmission
If the denial is correctable, the claim is updated and resubmitted. Timeliness matters. Most payers have strict appeal deadlines.
Appeals and Follow-Up
If the denial is disputed, a formal appeal is submitted with supporting documentation. Strong appeals depend on accurate records and clear communication.
Common Causes of Claim Denials

The top causes of denials are often preventable.
Below are frequent reasons organizations experience medical denial issues:
- Incorrect patient information
- Coding errors or mismatched diagnosis codes
- Missing prior authorization
- Insufficient documentation
- Services not covered under the patient plan
Understanding these patterns is central to effective claims denial management.
Denials Management in Medical Billing
Denials management in medical billing requires coordination between clinical staff, coders, and billing teams. It is not only a back-office function.
Front desk staff must verify insurance eligibility. Providers must document clearly. Coders must assign accurate codes. Billing teams must monitor submission accuracy. When one area fails, denials increase.
A study published by the National Library of Medicine at ncbi.nlm.nih.gov discusses how documentation and coding accuracy directly influence reimbursement outcomes in healthcare systems. This reinforces the importance of coordination across departments.
Preventing Denials Before They Happen
Effective denial management is proactive. Prevention reduces administrative workload and improves cash flow.
Key prevention strategies include:
Strong Documentation Standards
Clear and complete clinical documentation supports medical necessity and coding accuracy.
Accurate Coding Practices
Coders must stay updated with payer policies and regulatory changes. Small coding errors often lead to larger reimbursement problems.
Eligibility Verification
Insurance coverage must be confirmed before services are provided.
Authorization Tracking
Prior authorization requirements should be verified and documented before procedures.
Continuous Staff Training
Ongoing education ensures teams remain compliant with evolving payer guidelines.
Role of Denial Management Services
Some organizations use denial management services to strengthen internal processes. These services focus on tracking trends, improving appeals, and identifying root causes.
They often use data analytics to uncover patterns that may not be obvious in daily operations. However, whether managed internally or externally, the foundation remains the same. Clear workflows. Accurate documentation. Timely follow-up.
Financial Impact of Poor Denials Management
- Unresolved denials reduce cash flow and delay reimbursement.
- High denial rates increase days in accounts receivable.
- Administrative workload rises due to repeated claim corrections and follow-ups.
- Staff productivity declines when teams focus on rework instead of new submissions.
- Persistent denial patterns may increase compliance risks and audit exposure.
Connecting Denials Management to Revenue Performance
- Faster claim corrections improve reimbursement timelines.
- Denial trend tracking helps prevent recurring billing errors.
- Strong documentation reduces payer disputes.
- Accurate coding improves first pass claim acceptance rates.
- Structured denial workflows strengthen overall revenue cycle efficiency.
Conclusion
Denials management is not just about correcting rejected claims. It is a strategic function within revenue cycle operations. By identifying root causes, improving documentation, strengthening coding accuracy, and monitoring denial trends, healthcare organizations can reduce revenue loss and improve financial performance.
When managed effectively, denials management transforms payment disruptions into opportunities for operational improvement.
Frequently Asked Questions
What is denial management in healthcare?
Denials management in healthcare is the process of identifying, analyzing, correcting, and preventing claim denials to protect reimbursement and maintain financial stability.
What is a medical denial?
A medical denial occurs when a payer refuses to reimburse a claim due to documentation issues, coding errors, eligibility problems, or policy violations.
How does denial coding help?
Denial coding categorizes the reason for rejection. It helps organizations identify recurring problems and implement targeted improvements.
Why is denial management important in RCM?
Denial management in RCM protects cash flow, reduces administrative workload, and improves compliance by addressing claim issues systematically.
Can denied claims be recovered?
Yes. Many denied claims can be corrected and resubmitted or appealed within payer deadlines if proper documentation supports the service.








